By the time many people hit their 40s, the mirror starts telling a story of accumulated sun exposure: a few scattered dark patches, a couple of “age spots” on the back of the hands, and the sudden realization that those once-unseen flecks aren’t fading on their own.
Sun-induced pigmentation, such as age spots (also called solar lentigines), is so common that they’re considered a hallmark of photodamage, appearing in up to 90% of people as they age, especially in areas frequently exposed to the sun. These spots may not be dangerous, but they can make the skin look older or uneven, and they often prompt the question – What can I do to reverse them without trading one problem for another?
This article walks you through what age spots are, how they differ from potentially serious skin conditions like skin cancer, the most effective treatments (from creams to laser therapy), and how to protect your complexion so the spots don’t deepen or return. If you’ve ever hesitated to see a dermatologist, this is a little guide to confident, informed action.

What Are Age Spots and Why Do They Appear?
Age spots (sometimes called liver spots or sunspots) are small, flat, darker areas on the skin caused by localized overproduction of pigment (melanin) from years of sun exposure and ultraviolet (UV) radiation. They most often show up on skin that gets the most sun: the face, hands, shoulders, and arms. The technical term for them when due to solar damage is solar lentigines. They are a form of hyperpigmentation, meaning certain patches have more pigment than the surrounding skin.
The deeper cause is cumulative DNA damage to melanocytes (the pigment-producing cells) from UVA and UVB rays; over time, they cluster and produce excess melanin in spots instead of distributing it evenly. Fairer skin types often show age spots earlier, but any type of skin can develop them if repeatedly exposed to the sun without adequate sun protection.
Certain types of skin and individual predispositions amplify the risk:
- Fairer skin tones, especially those with a tendency to freckle or burn easily, are more likely to develop age spots earlier, because their melanocyte response to UV is more reactive and less diffuse.
- Genetic factors and existing skin conditions (like a history of frequent sunburns, or in rare cases, disorders such as xeroderma pigmentosum) can accelerate their appearance or lead to earlier onset.
- Hormonal influences (while more classically tied to melasma) can modulate pigmentation pathways and sometimes confuse the clinical picture, especially when multiple forms of dark spots are present.
- Chronic inflammation can cause post-inflammatory hyperpigmentation that coexists or overlaps with age spots, making the visual pattern more complex
Because several pigmentary disorders can look similar at a glance, it helps to distinguish age spots (solar lentigines) from their common lookalikes:
Freckles are typically smaller, often fade without intervention, and have a strong genetic component; they darken transiently with sun exposure but don’t usually persist or enlarge the way age spots do.
Melasma presents as larger, often symmetric patches and is driven more by hormonal and vascular factors in addition to sun, making its distribution and treatment distinct.
Other lentigines (e.g., those from phototherapy or rare syndromes) and benign lesions like seborrheic keratoses can mimic the look, which is why a brief evaluation by a dermatologist to confirm the diagnosis is wise before pursuing cosmetic fading.
Prevention (by protecting your skin consistently from UV with broad-spectrum sunscreen and limiting peak sun exposure) slows or halts new spots, while understanding the biology helps tailor the most effective fading or removal strategy.
Age Spots vs. Skin Cancer — What You Must Know
One of the most important early steps is distinguishing benign age spots from more serious concerns like skin cancer. Some growths, such as actinic keratoses, seborrheic keratoses, and certain melanomas, can mimic or coexist with age spots. Trying to fade or cover a spot without knowing what it is can delay diagnosis if the spot is malignant.
That’s why a timely evaluation by a qualified dermatologist is critical. A dermatologist like Orah Dermatologist can visually assess spots, and if anything is suspicious, biopsy it; when caught early, skin cancer is highly treatable.
Red flags that warrant immediate professional evaluation:
- Rapid change in size, color, or shape
- Irregular borders or multiple colors
- Itching, bleeding, or crusting
- A spot that looks markedly different from others (the “ugly duckling” sign)
Early triage keeps you safe and ensures that any cosmetic treatment doesn’t obscure a serious diagnosis.
Prevention: Protect Your Skin to Stop More Spots from Appearing
The most effective way to “remove” age spots is to prevent new ones. Sun damage is cumulative, so daily habits matter. Preventing age spots is far more effective and less expensive than treating them after they form.
Since most age spots are the visible result of cumulative sun exposure and ultraviolet (UV) damage, a disciplined prevention routine both slows new spots appearing and helps preserve any improvements from treatments. Here’s how to proactively protect your skin and stop existing dark spots or hyperpigmentation from darkening or recurring.
1. Daily, Non-Negotiable Sun Protection
Broad-spectrum sunscreen is the foundation. “Broad-spectrum” means it shields against both UVA (aging) and UVB (burning) rays, both contribute to pigment dysregulation that causes age spots.
Apply every day, even on cloudy or “indoor” days. UV rays penetrate clouds and reflect off surfaces; incidental exposure to the sun times (e.g., commuting, near windows) adds up. Use SPF 30 or higher. SPF measures UVB protection; higher numbers give incrementally more defense, but consistent application matters more than a single high number.
Reapply at least every two hours when outdoors, and immediately after swimming or sweating. Sunscreen wears off; failure to reapply is one of the most common reasons protection fails. Use about a nickel-sized amount for the face and a shot-glass worth for the body. Many people underapply, leaving gaps in coverage.
Common mistakes that undermine sun protection:
- Skipping sunscreen on “short” outings.
- Not reapplying after sweating or being in water.
- Using an expired product or one that’s been sitting in a hot car (efficacy degrades).
- Assuming makeup with SPF is enough, most people don’t apply it thickly enough for full protection.
Prefer mineral (physical) filters like zinc oxide or titanium dioxide if you are prone to hyperpigmentation; they sit on top of the skin, scatter UVA/UVB (and some visible light), and are less irritating for sensitive or melanin-rich skin. Tinted mineral sunscreens also help block visible light, which can exacerbate pigmentation.
Apply sunscreen as the last step of your morning skincare (after serums but before makeup), and wait ~15 minutes before sun exposure. Broad-spectrum sunscreen every day.
2. Wear Protective Clothing And Accessories
Wide-brim hats, UPF-rated clothing, and sunglasses shield skin that sunscreen might miss. Avoid peak sun hours (roughly 10 a.m – 4 p.m.) when ultraviolet intensity is highest.
Sunscreen is critical, but it works best in combination with physical defenses:
- Protective clothing: Look for garments with UPF ratings; tightly woven fabrics and long sleeves block much of the UV spectrum.
- Wide-brimmed hats shield the face, neck, and ears, common sites for age spots.
- Sunglasses with UV protection help protect the delicate periorbital skin, where pigmentation and premature aging also show.
- Seek shade during peak UV hours (typically 10 a.m. to 4 p.m.), or plan outdoor activities earlier or later in the day to reduce the cumulative UV dose.
Consistent sun protection not only prevents new age spots but also preserves and prolongs results from treatments
3. Behavior and Lifestyle Adjustments
Avoid tanning beds. Artificial ultraviolet exposure accelerates skin aging, increases uneven pigmentation, and raises the risk for skin cancer. Be cautious with reflective environments. Water, sand, snow, and even pavement bounce UV rays back onto skin, intensifying exposure.
Monitor cumulative exposure. Small daily amounts of UV add up. Consider wearing a UV index tracking app or using wearable indicators if you spend significant time outside. Regular skin checks. Even while preventing new age spots, schedule periodic self-exams and professional evaluations so any new or changing lesions (including those that might mimic age spots) are assessed early by a dermatologist.
4. Supportive Skin Care to Reinforce Prevention
Some topical ingredients don’t just treat existing dark spots. They help fortify skin against future pigment disruption. Antioxidants like vitamin C (ascorbic acid) neutralize free radicals generated by UV that can trigger hyperpigmentation pathways.
Niacinamide helps regulate pigment transfer and improves barrier function, making skin more resilient to subtle UV insults. Retinoids (used carefully and usually at night) help cellular turnover so early pigment irregularities don’t settle, and in long-term use can diminish the visual impact of mild sun damage.
Important tips for topical use:
- Always layer sunscreen on top; many of these actives make skin more photosensitive.
- Start slowly (e.g., alternate nights) to gauge tolerance, especially with retinoids.
- Give products 8–12 weeks to show visible improvement. Pigment fading is gradual.
These actives are often combined with sunscreen and stabilizing agents to maximize tolerance and results. Over-the-counter products can work for mild discoloration, but for deeper or more persistent age spots, a dermatologist can prescribe medical-grade formulations or tailor combination regimens.
In-Office Skin Care Procedures For Age Spots
When topical treatments aren’t enough, clinical procedures can markedly improve or even remove age spots by resurfacing the skin, breaking up pigment, or promoting regeneration. Commonly used cosmetic and medical treatments include:
1. Chemical Peels
Chemical peels use acids (like glycolic, salicylic, or trichloroacetic acid) to exfoliate the top layers of the layer of skin, encouraging new, more evenly pigmented skin to emerge. Medium to deeper peels can target more stubborn age spots and are often performed in series for best results.
2. Microdermabrasion
A mechanical exfoliation that polishes the outermost skin layers. It’s gentler than deeper peels and best for mild discoloration or maintenance after other treatments. Results are subtle and cumulative.
3. Laser Therapy
Lasers selectively target pigment clusters. Depending on the device (e.g., Q-switched lasers, intense pulsed light (IPL), fractional lasers), they either break apart melanin visually or stimulate skin renewal. Laser therapy is often combined with topical agents before and after to prolong outcomes.
4. Cryotherapy
Freezing age spots with liquid nitrogen can cause the pigmented cells to slough off. It’s quick but must be calibrated so as not to cause hypopigmentation or textural changes.
Many dermatology practices (including comprehensive ones like Orah Dermatology) layer treatments, such as preconditioning with retinoids, a series of peels, followed by laser touch-ups, because combining modalities often gives a more even, durable glow.
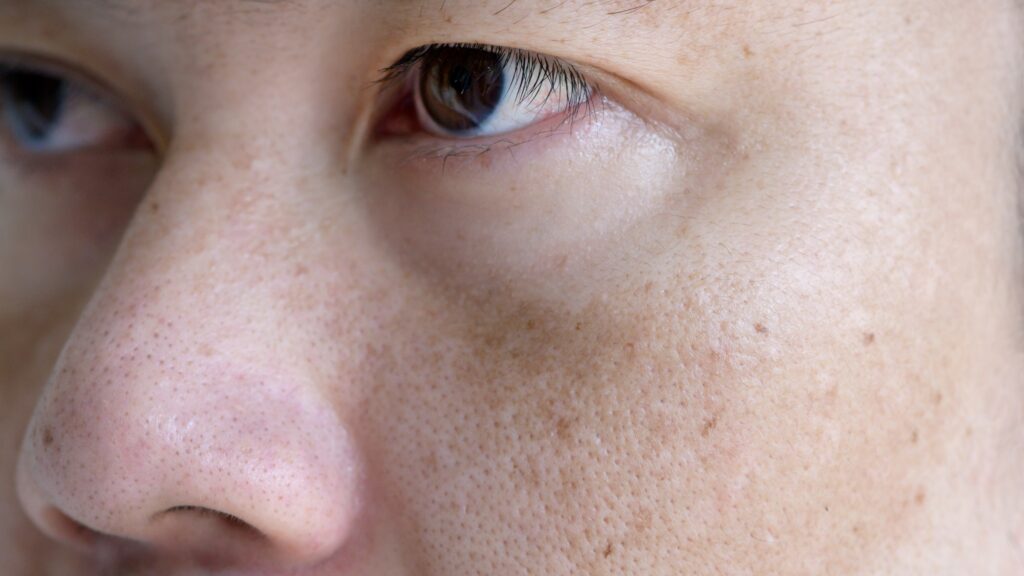
Special Considerations by Skin Type and Pigmentation Risk
People with darker skin tones can also develop age spots, but they may be more prone to post-inflammatory hyperpigmentation after aggressive treatments. That’s why a practical approach, starting with test spots, using lower-intensity procedures, and combining with brightening topicals, is critical to avoid unwanted darkening or uneven tone.
Those with a history of melasma or existing pigmentary disorders should prioritize sun protection and often benefit from mineral sunscreens, since these help block a broader spectrum (including visible light) that can trigger or worsen discoloration.
You should schedule a professional evaluation if:
- You have multiple age spots that bother you cosmetically.
- At-home treatments show limited improvement after 3 months.
- You’re unsure whether a spot is benign.
- You want a personalized plan combining prevention, topical therapy, and in-office procedures.
Peels are broadly resurfacing and can improve texture plus pigment; lasers can be more precise for isolated lentigines. A board-certified dermatologist will follow procedures to assess your skin type, depth of pigment, and healing capacity to recommend the right treatment path for you.
Age spots are a visible record of lived years and sun exposure, but they’re not a sentence. With informed prevention, the right combination of topical and professional treatments, and wise protection, you can significantly fade existing spots and keep future ones from stealing your skin’s radiance.
If you’re ready to fade age spots, protect your skin, or get a personalized plan tailored to your skin type, reach out to the experts at Orah Dermatology.
Schedule your consultation today through the easy online form, give the office a call, or send a message. Help is just a click away.